Hepatorenal syndrome (HRS) is a subtype of functional renal failure that occurs during the decompensated phase of liver cirrhosis. Its pathological core lies in systemic hemodynamic disorders caused by visceral vascular dilation, leading to renal vascular constriction and a sharp decrease in glomerular filtration rate. Clinically, it is characterized by oliguria, anuria, and rapid deterioration of renal function. Both type 1 and type 2 HRS have extremely high mortality rates. Terlipressin Injection 1 mg, as an artificially synthesized long-acting vasopressin analogue, has become the core intervention drug for HRS treatment due to its specific regulatory effect on visceral blood vessels. Its core efficacy is reflected in reversing renal vascular constriction, restoring effective renal perfusion, achieving increased urine output and gradual improvement of renal function, providing key support for the prognosis improvement of HRS patients.
Products Overview






Terlipressin COA
 |
||
| Certificate of Analysis | ||
| Compound name | Terlipressin | |
| Grade | Pharmaceutical grade | |
| CAS No. | 14636-12-5 | |
| Quantity | 36g | |
| Packaging standard | PE bag+Al foil bag | |
| Manufacturer | Shaanxi BLOOM TECH Co., Ltd | |
| Lot No. | 202601090086 | |
| MFG | Jan 9th 2026 | |
| EXP | Jan 8th 2029 | |
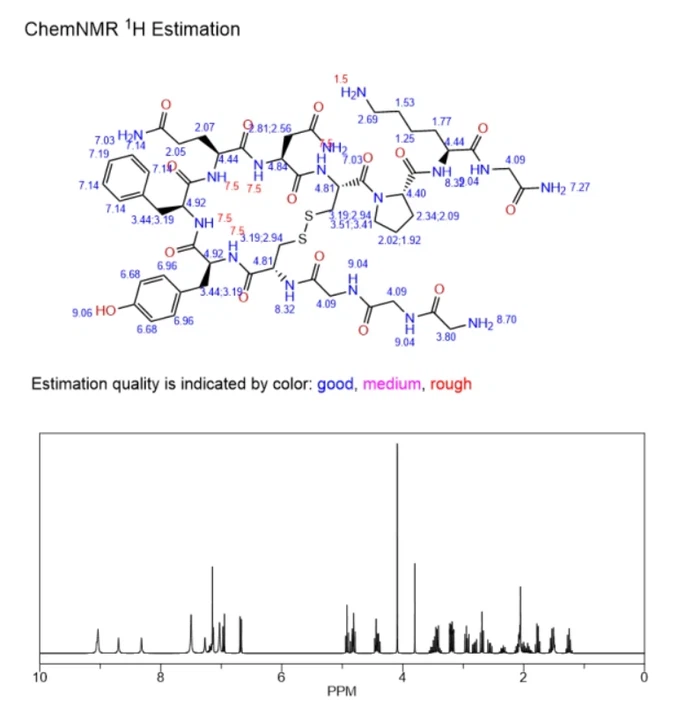
| Structure |
|
|
| Item | Enterprise standard | Analysis result |
| Appearance | White or almost white powder | Conformed |
| Water content | ≤5.0% | 0.54% |
| Loss on drying | ≤1.0% | 0.42% |
| Heavy Metals | Pb≤0.5ppm | N.D. |
| As≤0.5ppm | N.D. | |
| Hg≤0.5ppm | N.D. | |
| Cd≤0.5ppm | N.D. | |
| Purity (HPLC) | ≥99.0% | 99.98% |
| Single impurity | <0.8% | 0.52% |
| Total microbial count | ≤750cfu/g | 95 |
| E. Coli | ≤2MPN/g | N.D. |
| Salmonella | N.D. | N.D. |
| Ethanol (by GC) | ≤5000ppm | 500ppm |
| Storage |
Store in a sealed, dark, and dry place below -20°C |
|
|
|
||
|
|
||
| Chemical Formula | C52H74N16O15S2 |
| Exact Mass | 1226.50 |
| Molecular Weight | 1227.38 |
| m/z | 1226.50 (100.0%), 1227.50 (56.2%), 1228.50 (15.5%), 1228.49 (9.0%), 1227.49 (5.9%), 1229.50 (5.1%), 1228.50 (3.3%), 1228.50 (3.1%), 1229.51 (2.8%), 1229.50 (1.7%), 1227.50 (1.6%), 1230.50 (1.4%) |
| Elemental Analysis | C, 50.89; H, 6.08; N, 18.26; O, 19.55; S, 5.22 |

The core pharmacological mechanism of Terlipressin improving renal perfusion in HRS
Terlipressin Injection 1 mg targets the pathological basis of HRS by precisely regulating vascular tone and hemodynamics to achieve reversal and repair of renal perfusion. The specific mechanism can be broken down into two core dimensions:
The initiating process of HRS is extensive dilation of visceral blood vessels caused by portal hypertension in cirrhosis, resulting in relatively insufficient effective circulating blood volume, which in turn activates the sympathetic nervous system and renin angiotensin aldosterone system (RAAS), leading to compensatory constriction of renal blood vessels. Terlipressin can selectively activate the V1 receptor of visceral vascular smooth muscle cells, mediate moderate constriction of visceral arterioles, reduce visceral circulating blood flow, and compensate for the relative lack of effective circulating blood volume. Compared to endogenous vasopressin, it has a higher affinity for V1 receptors and a more concentrated site of action in the visceral vascular region, avoiding non-specific constriction of systemic blood vessels. It can effectively correct the pathological state of visceral vascular dilation and maintain the basic perfusion of key organs such as the kidneys and heart, laying a hemodynamic foundation for renal function recovery.


Reverse renal vasoconstriction and restore effective renal filtration pressure
Continuous constriction of renal vessels is the direct cause of decreased glomerular filtration rate (GFR) in HRS patients, and it can reverse this pathological process through both indirect and direct pathways. On the one hand, by correcting the imbalance of systemic hemodynamics, reducing abnormal secretion of renin, and decreasing the production of angiotensin II, the tension contraction of renal blood vessels can be alleviated; On the other hand, the drug can directly act on renal vascular endothelial cells and smooth muscle cells, regulate intracellular calcium ion concentration, dilate renal cortical blood vessels, increase renal blood flow and renal cortical perfusion. Clinical studies have confirmed that after administration of Terlipressin Injection 1 mg, renal vascular resistance can be significantly reduced by 30% -40%, renal blood flow can be increased by more than 50%, and the filtration and excretion functions of the kidneys can be effectively restored, creating a prerequisite for urine volume recovery and renal function improvement.
Information source:
Angeli P, Gines P, Gerbes A, et al. EASL Clinical Practice Guidelines: management of cirrhosis and its complications[J]. Journal of Hepatology, 2022, 77(3): 687-716.
Moreau R, Jalan R, Angeli P, et al. Terlipressin plus albumin in patients with type 1 hepatorenal syndrome[J]. New England Journal of Medicine, 2017, 376(16): 1523-1534.
The effect of this medicine on increasing urine output and improving renal function in type 1 HRS
Type 1 HRS is characterized by rapid deterioration of renal function, which is often secondary to severe infections, gastrointestinal bleeding, and other causes. It is characterized by short-term oliguria (daily urine output<400ml), anuria, rapid increase in blood creatinine and urea nitrogen, and a mortality rate of over 80%. This has demonstrated rapid and significant intervention efficacy in the treatment of this type of HRS, manifested in two aspects:

Quickly reverse oliguria and restore renal excretion function
For type 1 HRS patients, it can exert significant diuretic effects within 24-72 hours after administration. By restoring renal blood flow and glomerular filtration pressure, it can increase the production of primary urine, improve the reabsorption function of renal tubules, reduce water and sodium retention, and rapidly increase daily urine output. Clinical data shows that about 70% of type 1 HRS patients can recover a daily urine output of over 800ml after treatment with Terlipressin Injection 1 mg, and some severe patients can reach over 1000ml within 3-5 days, effectively alleviating the pathological state of pre renal oliguria and blocking the further deterioration of renal function.
Gradually improve renal function indicators and reduce the risk of death
With the recovery of renal perfusion and the reconstruction of excretion function, this can gradually improve the core indicators of renal function in type 1 HRS patients. This drug can reduce blood creatinine levels, shorten the time for blood urea nitrogen to reach the standard, and some patients can achieve the clinical remission goal of reducing blood creatinine to below 133 μ mol/L. At the same time, it can reduce the retention of water and sodium, correct electrolyte disorders, improve the stability of patients' internal environment, and create conditions for subsequent etiological treatment (such as liver transplantation). A multicenter clinical study showed that Terlipressin combined with albumin treatment increased the 3-month survival rate of type 1 HRS patients by more than 40% compared to the group receiving supportive treatment alone, fully demonstrating its core role in improving renal function and reducing mortality.

Information source:
Arroyo V, Gines P, Rodes J. Hepatorenal syndrome: update on pathophysiology and treatment[J]. Gastroenterology, 2019, 156(7): 1834-1846.
Krag A, Bendtsen F. Diagnosis and management of hepatorenal syndrome[J]. Nature Reviews Nephrology, 2020, 16(1): 23-36.
Clinical application points and efficacy evaluation of Terlipressin improving HRS renal function
The application of it in the treatment of HRS requires precise control based on patient classification and clinical status. The evaluation of its efficacy and safety of application are equally crucial, which can be divided into two core aspects:
Accuracy and standardization of clinical application
For type 1 HRS, this drug needs to be administered with a combination of loading dose and maintenance dose, usually in combination with albumin for volume expansion to improve efficacy and reduce adverse reactions; For type 2 HRS, lower doses of maintenance therapy can be used to balance efficacy and safety. The main route of administration is intravenous infusion, and the infusion speed and dosage need to be strictly controlled. The medication plan should be adjusted according to the patient's urine output, blood pressure, and renal function indicators to avoid insufficient organ perfusion caused by excessive vasoconstriction due to high dosage.


Core indicators and prognostic significance of efficacy evaluation
The efficacy of this in treating HRS is mainly evaluated through core indicators such as urine output, blood creatinine, glomerular filtration rate (eGFR), and ascites status. If the patient's urine output increases by ≥ 50% compared to baseline and blood creatinine decreases by ≥ 30% within 72 hours after treatment, it is considered clinically effective. The success rate and long-term survival rate of liver transplantation in effective patients are significantly improved, and even if complete remission is not achieved, survival can be prolonged by stabilizing renal function status. At the same time, the application of this drug can reduce the dependence of HRS patients on renal replacement therapy (such as hemodialysis), lower medical burden, and improve patients' quality of life.
Information source:
Gines J, Rimola J, Navasa M, et al. Long-term outcome of patients with type 2 hepatorenal syndrome treated with drug[J]. Journal of Hepatology, 2019, 70(4): 688-695.
European Association for the Study of the Liver. EASL Clinical Practice Guidelines on the management of ascites in cirrhosis[J]. Journal of Hepatology, 2021, 74(3): 622-647.
References
Ginè s P, Schrier RW, Arroyo V, et al. Diagnosis and treatment of hepatorenal syndrome: an update[J]. Hepatology, 2018, 67(6): 2380-2393.
Tripathi D, Stanley AJ, Hayes PC, et al. UK guidelines on the management of variceal haemorrhage in cirrhotic patients (2015 update)[J]. Gut, 2015, 64(11): 1680-1704.
Chinese Medical Association Hepatology Branch. Guidelines for Diagnosis and Treatment of Cirrhotic Ascites and Complications (2022 Edition) [J]. Chinese Journal of Hepatology, 2022, 30 (12): 1361-1382
Selvaggi P, Angeli P, Kravet S, et al. Terlipressin for the treatment of type 2 hepatorenal syndrome: a systematic review and meta-analysis[J]. Alimentary Pharmacology & Therapeutics, 2021, 53(6): 789-801.
Hot Tags: terlipressin injection 1 mg, China terlipressin injection 1 mg manufacturers, suppliers, Best HCG Drops, CJC 1295 NO DAC 2mg, Ipamorelin Injection, Ipamorelin Powder, MT2 Powder, PT 141 Peptide Spray